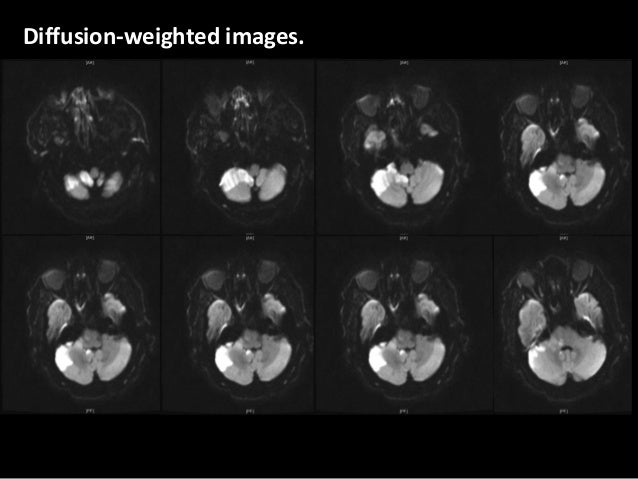
In the subacute phase of stroke, Horner’s syndrome, as well as orthostatic hypotension, was symptomatic of a sympathetic impairment, while tearing and ocular injection reflected a parasympathetic activation. In this area, descending fibers of the hypothalamospinal tract carry sympathetic innervation to the pericarotid plexus (Fig. In our patient, the ischemic lesion was located in the left posterior side of the upper medulla oblongata (Fig. Hypothalamospinal tract lies in dorsolateral medulla it is constituted by first order neurons responsible for orthosympathetic innervation of ipsilateral half face and body and projects to peri-acqueductal gray matter, thus activating the trigeminovascular system that is a well-known pain generator of headaches. Moreover, stereotactic hypothalamic stimulation has been successfully used in drug-resistant patients, indirectly confirming the hypothalamic involvement in TACs’ pathophysiology. Experimental studies with functional MRI and PET showed hypothalamic activation during TACs attack. The hypothalamus, via the hypothalamospinal tract, is a regulatory centre for integration of sympathetic and parasympathetic systems. Central nervous system lesions can rarely present with cluster-like or SUNCT-like symptomatology. TACs are primary headaches characterized by typical pain and autonomic features. The patient’s explicit and signed consent for publishing this case was obtained. The patient was still on therapy with verapamil 240 mg/day. Neurological examination showed left mild inferior facial palsy, dysesthesia in the first trigeminal branch territory, and ptosis left miosis as well as orthostatic hypotension was no longer present. Orthostatic position did not trigger pain exacerbation any longer. Pain and associated symptoms clinically resembled TACs: attacks occurred several times a day (3–6), twice a week, for about 15–30 min, with milder pain than in subacute phase, and persistence of tearing and conjunctival injection. Verapamil (240 mg/day) used on the basis of a previous report, successfully treated headache and vegetative phenomena but not Horner’s syndrome that partially recovered after 10 days.Īt the 3-month follow-up visit, headache characteristics had changed since the subacute phase of stroke. However, it never prevented pain flares induced by standing up. Indomethacin (100 mg/day), administered at the onset of pain for 3 days, slightly improved pain severity but not associated symptoms. These features were suggestive of autonomic dysfunction.Ĭommon NSAIDs and pregabalin (150 mg/day) were ineffective in controlling pain. Arterial blood pressure evaluation demonstrated orthostatic hypotension, changing from 150/90 mmHg in supine position to 115/80 mmHg in orthostatic position, persisting after 1, 3, and 5 min. Pain exacerbations lasted as long as the patient stood and were associated with ipsilateral conjunctival injection, lacrimation, and nostril blockage (Fig. Brain MRI revealed a small subacute left dorsolateral medullary infarction.įew days later, the continuous pressure-like pain had resolved, but the patient experienced dramatic pain flares triggered exclusively when moving from clinostatic to orthostatic position, which he could hardly maintain. Cranial CT scan and duplex ultrasound of cerebral and neck vessels were normal. However, the patient showed limb ataxia with left lateropulsion, but co-ordination and other cerebellar functions were intact. Muscular tone and strength were conserved deep tendon reflexes were normal and symmetrical signs of pyramidal tract involvement were absent. Neurological examination revealed hypacusia on the left side, weaker corneal reflex, Horner’s syndrome, inferior facial hyposthenia and hypoesthesia, cold-like paresthesia in the first trigeminal branch territory, and no other signs of cranial nerves involvement or papillary edema. One month earlier, he arbitrarily stopped aspirin (100 mg/day) and ticlopidine (250 mg/day) intake. His medical history included hypertension, diabetes, myocardial infarction, cistectomy for bladder tumor, and an asymptomatic cerebral meningioma in left parietal area with the dimension of 20 × 16 mm, never surgically treated. A 67-year-old Caucasian male was admitted to our hospital for left orbital, retro-orbital and temporal continuous pressure-like pain of moderate intensity, and gait disorder that suddenly started 15 days earlier.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
